What is fetal monitoring during pregnancy, and why is it necessary?
Fetal monitoring during pregnancy is a crucial aspect of prenatal care that involves assessing the well-being and development of the unborn baby. This process is typically conducted through various methods to track the baby’s heart rate and movements, providing valuable information to healthcare professionals about the fetus’s health and ensuring a safe and healthy pregnancy.
Importance of Fetal Monitoring
- Early Detection of Complications: Fetal monitoring helps in the early detection of potential complications, such as fetal distress, oxygen deprivation, or abnormal heart rates. Timely identification allows healthcare professionals to take appropriate measures to address these issues.
- Monitoring High-Risk Pregnancies: In high-risk pregnancies, where conditions such as gestational diabetes, preeclampsia, or multiple pregnancies are present, continuous fetal monitoring is essential to ensure the well-being of both the mother and the baby.
- Assessment of Fetal Development: Fetal monitoring allows healthcare professionals to assess the baby’s growth, development, and overall health throughout the pregnancy. This information aids in developing an appropriate care plan and making decisions about the timing and mode of delivery.
- Reducing the Risk of Stillbirth: Continuous monitoring helps identify signs of fetal distress, reducing the risk of stillbirth by allowing timely medical interventions or adjustments in the management of the pregnancy.
Regular monitoring is particularly crucial in high-risk pregnancies, guiding medical interventions and promoting optimal fetal development throughout the gestational period.
Table of Contents
How is fetal well-being monitoring performed, and when does it typically start?
Fetal well-being monitoring is performed through various methods to assess the health and development of the unborn baby during pregnancy. The timing of these monitoring techniques can vary, but they generally start during the second trimester and continue through the third trimester. Here’s an overview of how fetal well-being monitoring is performed and when it typically begins:
1. Ultrasound Examinations
- Timing: Ultrasound examinations are commonly performed throughout the pregnancy, but a detailed anatomy scan is typically done around 18-20 weeks.
- Procedure: A gel is applied to the mother’s abdomen, and a transducer is moved over the belly to emit sound waves. The echoes create an image of the fetus, allowing healthcare providers to assess the baby’s growth, anatomy, and the placenta.
2. Doppler Ultrasound
- Timing: Doppler ultrasound for monitoring the fetal heartbeat can be performed as early as the first trimester and throughout the pregnancy.
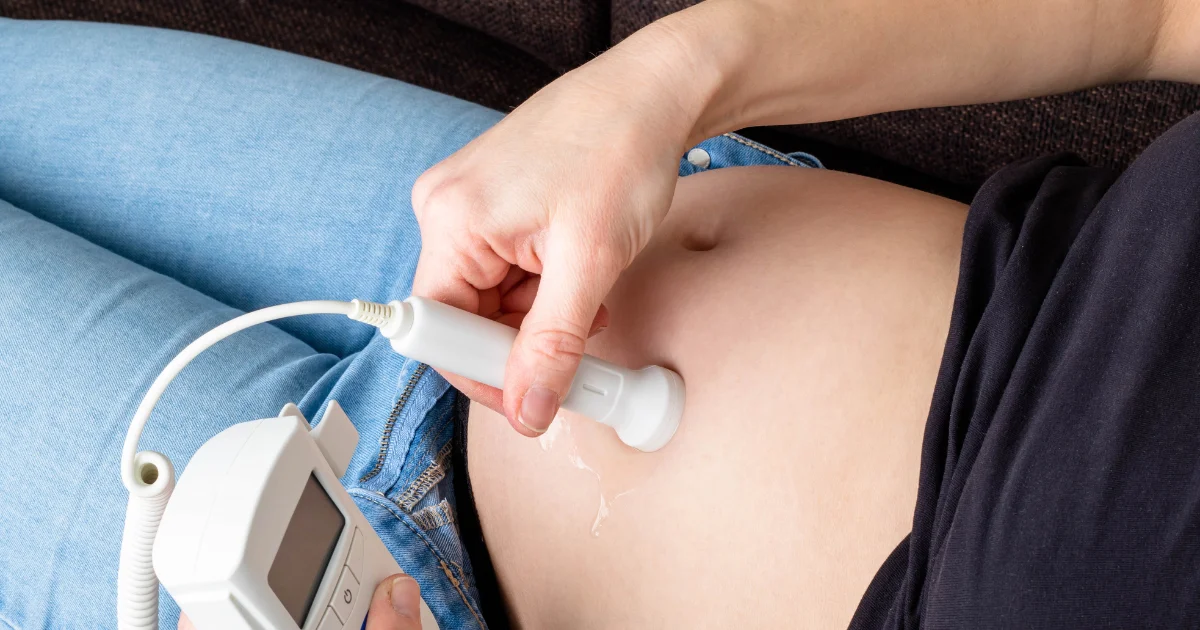
- Procedure: A Doppler device is used to listen to the baby’s heartbeat. This non-invasive method helps assess the rhythm and rate of the fetal heart, providing information about the baby’s well-being.
3. Non-Stress Test (NST)
- Timing: Typically performed in the third trimester, starting around 28 weeks, or earlier if there are specific concerns.
- Procedure: The mother is connected to a fetal monitor, which records the baby’s heart rate in response to its movements. An increase in heart rate during movement is a positive sign of fetal well-being.
4. Biophysical Profile (BPP)
- Timing: BPP is usually performed in the third trimester, often starting around 28 weeks or later.
- Procedure: BPP combines ultrasound and NST. It assesses fetal breathing movements, muscle tone, body movements, amniotic fluid levels, and the baby’s heart rate response to movements.
5. Electronic Fetal Monitoring (EFM)
- Timing: EFM is commonly used during labor and delivery.
- Procedure: Sensors are attached to the mother’s abdomen to monitor both contractions and the baby’s heart rate continuously. This helps assess fetal well-being during the stress of labor.
It’s important to note that the timing and frequency of fetal monitoring may be adjusted based on the individual circumstances of the pregnancy. High-risk pregnancies, maternal age, medical history, and other factors may influence the healthcare provider’s decision on when and how often monitoring should occur. Regular prenatal check-ups, which typically start in the first trimester, also involve monitoring the mother’s overall health and the progress of the pregnancy.
Also read: A Comprehensive Guide to Fetal Monitoring During Labor
What is Electronic Fetal Monitoring (EFM), and how does it work?
Electronic Fetal Monitoring (EFM) is a medical procedure used during pregnancy and labor to monitor the heartbeat of the fetus and the contractions of the mother’s uterus. This monitoring system plays a crucial role in assessing the unborn baby’s well-being and providing valuable information to healthcare professionals, helping them make informed decisions about the management of labor and delivery.
How EFM Works
1. Sensors Placement: EFM involves attaching sensors externally to the mother’s abdomen. These sensors have transducers that detect and record the electrical signals generated by the fetal heart and uterine contractions.
2. Fetal Heart Rate Monitoring: The primary function of EFM is to monitor the fetal heart rate. The sensor placed on the mother’s abdomen captures the electrical impulses generated by the baby’s heart. This data is then transmitted to the monitoring equipment.
3. Uterine Contraction Monitoring: In addition to tracking the fetal heart rate, EFM also monitors uterine contractions. A separate sensor measures the frequency and duration of contractions by detecting changes in the electrical activity of the uterine muscles.
4. Data Display: The information collected by the sensors is displayed on a monitor or printed on a graph. The fetal heart rate is typically represented as a continuous line, and uterine contractions are recorded as spikes or waves on the same graph.
5. Interpretation by Healthcare Providers: Healthcare providers interpret the data to assess the relationship between the fetal heart rate and uterine contractions. Normal patterns indicate a healthy, well-oxygenated fetus, while deviations may signal potential issues such as fetal distress.
6. Identification of Variability and Decelerations: EFM allows healthcare professionals to identify important patterns in the fetal heart rate, including variability (fluctuations in the heart rate) and decelerations (temporary decreases in the heart rate). The absence of variability or certain types of decelerations may indicate a need for closer monitoring or intervention.
7. Informed Decision-Making: The information obtained from EFM assists healthcare providers in making timely and informed decisions during labor. If signs of fetal distress are observed, interventions may be recommended, such as changes in the mother’s position, administration of oxygen, or, in more critical situations, an expedited delivery through methods like cesarean section.
By continuously monitoring the fetal heart rate and uterine contractions, healthcare professionals can identify potential issues and take appropriate actions to ensure a safe and healthy delivery for both the mother and the baby.
Why is CTG done during pregnancy?
Cardiotocography (CTG), also known as electronic fetal monitoring, is done during pregnancy to assess the well-being of the unborn baby. This non-invasive monitoring technique involves recording fetal heart rate and uterine contractions to provide valuable information to healthcare providers. Here are the primary reasons why CTG is performed during pregnancy:
1. Monitoring Fetal Heart Rate: The main purpose of CTG is to continuously monitor the fetal heart rate. Changes in the heart rate can indicate the baby’s response to various factors, such as oxygen levels, and may provide insights into the overall well-being of the fetus.
2. Assessing Fetal Oxygenation: By monitoring the fetal heart rate patterns, CTG helps healthcare providers assess the adequacy of oxygen supply to the baby. Deviations from normal heart rate patterns may signal potential issues, such as fetal distress or oxygen deprivation.
3. Detecting Fetal Distress: CTG is particularly important in identifying signs of fetal distress during pregnancy. Fetal distress may occur when the baby is not receiving enough oxygen or nutrients, and the monitoring helps healthcare providers intervene promptly to address the underlying cause.
4. High-Risk Pregnancies: In pregnancies considered high-risk due to factors such as maternal age, medical conditions, or complications, CTG is often used as a routine monitoring tool. It allows healthcare providers to closely observe the fetal well-being and take preventive measures if necessary.
5. During Labor: CTG is commonly used during labor to assess the baby’s response to uterine contractions. This real-time monitoring helps healthcare professionals make informed decisions about the management of labor, including the timing of interventions or the need for a cesarean section.
6. Guiding Interventions: CTG provides crucial information that guides healthcare providers in making decisions about interventions during pregnancy and labor. If abnormalities in the fetal heart rate are detected, adjustments can be made to optimize conditions for the baby, such as changing the mother’s position, administering oxygen, or considering expedited delivery.
7. Reducing the Risk of Complications: Early detection of potential issues through CTG allows for timely interventions, reducing the risk of complications such as birth asphyxia or stillbirth. This proactive approach contributes to better outcomes for both the mother and the baby.
In summary, CTG is performed during pregnancy to continuously monitor the fetal heart rate and uterine contractions, providing valuable information about the well-being of the unborn baby. It is an essential tool in the management of pregnancies, particularly in high-risk situations, and plays a crucial role in ensuring a safe and healthy delivery.
What are the 3 ways to monitor the unborn fetus?
There are several ways to monitor the unborn fetus during pregnancy, and three common methods include:
1. Doppler Ultrasound
- Procedure: Doppler ultrasound involves using a handheld device that emits high-frequency sound waves. These waves bounce off moving blood cells in the umbilical cord and fetal heart, creating audible signals.
- Purpose: It is primarily used to listen to and monitor the fetal heartbeat. Doppler ultrasound is a non-invasive and safe method that allows healthcare providers to assess the rhythm and rate of the fetal heart throughout the pregnancy.
2. Electronic Fetal Monitoring (EFM)
- Procedure: EFM is typically used during labor and delivery. It involves attaching sensors to the mother’s abdomen to monitor both the fetal heart rate and uterine contractions continuously.
- Purpose: EFM provides real-time information about the baby’s heart rate patterns in response to contractions, helping healthcare providers assess fetal well-being and make informed decisions during labor.
3. Ultrasound Examinations
- Procedure: Ultrasound examinations utilize sound waves to create images of the developing fetus. A gel is applied to the mother’s abdomen, and a transducer is moved over the belly to capture images.
- Purpose: Ultrasounds serve various purposes, including assessing fetal growth, anatomy, and development. They can be performed at different stages of pregnancy, with a detailed anatomy scan often conducted around 18-20 weeks to check for any abnormalities.
These monitoring methods provide valuable information about the fetus’s health and development at different stages of pregnancy, allowing healthcare professionals to detect any potential issues and ensure the well-being of both the mother and the unborn baby. The choice of monitoring method may depend on factors such as the stage of pregnancy, the presence of risk factors, and the specific information needed by healthcare providers.
Are there any risks associated with fetal monitoring procedures during pregnancy?
While fetal monitoring procedures are generally considered safe and routine, like any medical intervention, there are some potential risks and considerations associated with certain monitoring methods. It’s important to note that the benefits of fetal monitoring often outweigh the risks, especially in situations where there are concerns about the well-being of the unborn baby. Here are some considerations:
1. Ultrasound
- Potential Risks: Diagnostic ultrasound, used for imaging and assessing fetal development, is generally considered safe. However, prolonged exposure to high-intensity ultrasound or unnecessary use should be avoided. Some studies suggest a correlation between extensive ultrasound exposure and low birth weight, but more research is needed to establish causation.
- Guidance: Ultrasounds are usually performed by trained professionals following established guidelines. Routine ultrasounds for monitoring fetal development are generally considered safe.
2. Doppler Ultrasound
- Potential Risks: Doppler ultrasound for fetal heart rate monitoring is considered safe, but extended and frequent use should be avoided. Prolonged exposure to ultrasound waves may generate heat, and while this is typically minimal, the effects of long-term exposure are not well understood.
- Guidance: Doppler ultrasound is commonly used in prenatal care, and healthcare providers follow recommended guidelines to minimize any potential risks.
3. Electronic Fetal Monitoring (EFM)
- Potential Risks: The use of EFM during labor is generally safe. However, it may lead to an increased rate of interventions, such as cesarean sections, if the monitoring suggests concerns that may not be present. Continuous monitoring may also limit the mother’s mobility during labor.
- Guidance: EFM is carefully employed based on clinical indications, and healthcare providers make decisions on interventions based on a comprehensive assessment of the mother’s and baby’s well-being.
It’s crucial for healthcare providers to carefully weigh the benefits and risks of fetal monitoring procedures, taking into account the specific circumstances of each pregnancy. Routine monitoring is often recommended, especially in high-risk pregnancies, to ensure the well-being of both the mother and the unborn baby. If there are concerns about the potential risks associated with monitoring procedures, individuals should discuss them with their healthcare provider for personalized guidance.
What are the common indications for continuous fetal monitoring?
Continuous fetal monitoring is often employed during pregnancy, labor, and delivery in specific situations where there is a need for closer observation of the unborn baby’s well-being. Common indications for continuous fetal monitoring include:
1. High-Risk Pregnancies
- Explanation: Continuous fetal monitoring is frequently recommended in pregnancies considered high-risk due to factors such as maternal age, multiple pregnancies (twins or more), gestational diabetes, hypertension, or pre-existing medical conditions.
- Rationale: Monitoring helps healthcare providers closely observe fetal well-being and respond promptly to any signs of distress or complications.
2. Preterm Labor
- Explanation: Continuous monitoring is often used in cases of preterm labor to assess the fetal heart rate and uterine contractions and detect any signs of distress.
- Rationale: Preterm infants may face increased risks, and monitoring helps in making timely decisions to optimize outcomes.
3. Induction or Augmentation of Labor
- Explanation: When labor is induced or augmented using medications, continuous fetal monitoring is commonly employed to ensure that the baby responds appropriately to contractions.
- Rationale: Induced or augmented labor may place stress on the baby, and continuous monitoring helps in adjusting interventions as needed.
4. Suspected Fetal Distress
- Explanation: If there are concerns about the baby’s well-being, such as decreased fetal movements, abnormal maternal blood pressure, or signs of placental insufficiency, continuous monitoring may be initiated.
- Rationale: Continuous monitoring allows for real-time assessment of the fetal heart rate patterns and helps identify signs of distress.
5. Abnormalities in Previous Labors
- Explanation: If a woman has experienced complications or abnormalities in previous labors, such as a history of fetal distress, continuous fetal monitoring may be recommended in subsequent pregnancies.
- Rationale: Past complications may indicate an increased risk of recurrence, and monitoring helps in early detection and intervention.
6. Multiple Pregnancies
- Explanation: Women carrying twins, triplets, or more are often monitored continuously to assess the well-being of each fetus individually.
- Rationale: Multiple pregnancies have an increased risk of complications, and continuous monitoring helps ensure that each baby is tolerating the labor process well.
7. Prolonged Labor
- Explanation: If labor is prolonged, continuous monitoring may be employed to evaluate the fetal response to prolonged contractions.
- Rationale: Prolonged labor may lead to fetal distress, and monitoring helps healthcare providers make informed decisions about the management of labor.
It’s important to note that the decision to use continuous fetal monitoring is individualized based on the specific circumstances of each pregnancy. Healthcare providers carefully assess risk factors and indications to determine the most appropriate approach to monitoring that will ensure the safety and well-being of both the mother and the unborn baby.
How often should fetal monitoring be performed during pregnancy?
The frequency of fetal monitoring during pregnancy depends on several factors, including the gestational age, the presence of risk factors, and the overall health of the pregnancy. In general, there are specific milestones and timeframes during which fetal monitoring is routinely performed. Here is an overview:
1. First Trimester
- Monitoring: During the first trimester, routine prenatal care focuses on confirming the pregnancy, assessing the mother’s health, and establishing a baseline for the pregnancy.
- Tests and Examinations: This period often involves an initial ultrasound to confirm the gestational age and check for the presence of a viable embryo or fetus. Blood tests may also be conducted to assess the mother’s health and screen for certain conditions.
2. Second Trimester
- Monitoring: In the second trimester, routine prenatal visits become more frequent.
- Tests and Examinations: An anatomy ultrasound scan is commonly performed around 18-20 weeks to assess fetal development, check for any abnormalities, and confirm the gender if desired. Additional blood tests may be conducted to screen for genetic disorders.
3. Third Trimester
- Monitoring: Fetal monitoring becomes more regular in the third trimester.
- Tests and Examinations: Depending on the healthcare provider’s recommendations and the presence of risk factors, additional ultrasounds may be performed. Non-stress tests (NST) or biophysical profile (BPP) tests may be initiated, especially in high-risk pregnancies.
4. High-Risk Pregnancies
- Monitoring: In high-risk pregnancies, more frequent and intensive monitoring may be necessary throughout all trimesters.
- Tests and Examinations: High-risk pregnancies, due to factors such as advanced maternal age, multiple pregnancies, or pre-existing medical conditions, often involve additional ultrasounds, NSTs, or BPP tests to closely monitor fetal well-being.
5. During Labor
- Monitoring: Continuous fetal monitoring is typically initiated during labor, especially in hospitals or birthing centers.
- Tests and Examinations: Electronic fetal monitoring (EFM) is commonly used to assess the fetal heart rate and uterine contractions during labor, providing real-time information for healthcare providers to make informed decisions.
Pregnant individuals need to attend regular prenatal check-ups as recommended by their healthcare provider. The frequency of monitoring can be adjusted based on the specific needs and circumstances of each pregnancy. Any concerns, changes in fetal movement, or unusual symptoms should be promptly reported to the healthcare provider for further evaluation. Regular and appropriate monitoring contributes to the overall well-being of both the mother and the unborn baby.
What happens if abnormalities are detected during fetal monitoring?
If abnormalities are detected during fetal monitoring, healthcare providers will take prompt and appropriate actions to address the concerns and ensure the well-being of both the mother and the unborn baby. The specific interventions may vary depending on the nature and severity of the abnormalities, but some common responses include:
1. Further Assessment: If abnormalities are noted in fetal heart rate patterns or other monitoring parameters, healthcare providers will conduct a more detailed assessment. This may involve additional tests, such as a biophysical profile (BPP) or a non-stress test (NST), to gather more information about the baby’s well-being.
2. Change in Maternal Position: Changing the mother’s position, such as moving from lying on her back to her side, can sometimes improve blood flow to the uterus and enhance fetal oxygenation. This simple adjustment may be attempted to see if it positively influences the fetal heart rate patterns.
3. Oxygen Administration: If there are signs of fetal distress, administering oxygen to the mother may help increase oxygen levels in her blood, thereby improving oxygen delivery to the baby. This is often done through a mask worn by the mother.
4. Intravenous (IV) Fluids: Intravenous fluids may be administered to the mother to improve hydration and blood flow, potentially enhancing fetal well-being. Adequate hydration is important for maintaining optimal blood volume and placental perfusion.
5. Medication Adjustment: If contractions are causing stress to the fetus, medications to slow down or stop contractions (tocolytics) may be considered. Conversely, if contractions are too weak, medications to stimulate contractions (oxytocin) may be administered.
6. Emergency Cesarean Section: In severe cases of fetal distress or if interventions do not improve the situation, an emergency cesarean section may be performed. This is a surgical procedure to deliver the baby quickly and safely.
7. Close Monitoring and Observation: Continuous monitoring allows healthcare providers to closely observe how the baby responds to interventions. Depending on the situation, monitoring may be extended to ensure the baby’s well-being during and after the implementation of corrective measures.
It’s important to note that the response to abnormalities detected during fetal monitoring will be individualized based on the specific circumstances of each case. The healthcare team will consider factors such as gestational age, maternal health, and the nature of the abnormalities when deciding on the most appropriate course of action. The goal is to address any concerns promptly and optimize conditions for a safe and healthy delivery. Effective communication between the healthcare provider and the pregnant individual is crucial during these situations.
Is fetal monitoring necessary for low-risk pregnancies?
The necessity of fetal monitoring for low-risk pregnancies is a topic that has been debated in the field of obstetrics. While continuous fetal monitoring may not be routinely recommended for all low-risk pregnancies, healthcare providers often individualize their approach based on various factors. Here are some considerations:
1. Routine Prenatal Care: In low-risk pregnancies, routine prenatal care involves regular check-ups, including physical examinations, blood tests, and ultrasounds. These appointments allow healthcare providers to monitor the overall health of both the mother and the unborn baby.
2. Intermittent Fetal Monitoring: Low-risk pregnancies may not require continuous electronic fetal monitoring (EFM) during labor. Instead, intermittent monitoring, such as periodic checks with a handheld Doppler device or monitoring the baby’s heart rate after contractions, may be used.
3. Assessment of Risk Factors: Healthcare providers assess various factors to determine the level of risk associated with a pregnancy. If a pregnancy is truly low-risk, meaning there are no identified complications or concerns, continuous monitoring may be considered unnecessary.
4. Shared Decision-Making: The decision to use continuous fetal monitoring is often made collaboratively between the healthcare provider and the pregnant individual. Informed consent and shared decision-making allow individuals to be actively involved in the choices regarding their care.
5. Birth Setting: The choice of birth setting, such as a hospital, birthing center, or home, may influence the approach to fetal monitoring. Hospitals, where medical interventions are readily available, may have different monitoring practices compared to low-intervention birthing centers or home births.
6. Individualized Care Plans: Healthcare providers may develop individualized care plans based on factors such as maternal age, medical history, and preferences. Continuous fetal monitoring may be recommended if certain risk factors emerge during the pregnancy or labor.
It’s important to recognize that the definition of a low-risk pregnancy is not absolute and can vary. Additionally, recommendations may evolve based on emerging research and clinical guidelines. Continuous fetal monitoring is more commonly emphasized in high-risk pregnancies or situations where complications are anticipated. However, in certain cases, intermittent monitoring or minimal intervention may be considered appropriate for low-risk pregnancies.
Final Words
Pregnant individuals are encouraged to have open and informed discussions with their healthcare providers about the best approach to monitoring based on their individual circumstances, preferences, and the latest evidence-based practices. Regular prenatal care remains a cornerstone of ensuring the health and well-being of both the mother and the unborn baby.